|
Milk of calcium pleural collections have previously been reported following pleural tuberculosis and pleuropulmonary paragonimiasis, as well as in a bronchogenic cyst 2, 3, chemical analysis showing a colloidal suspension of calcium crystals. The presence of milk of calcium (calcium carbonate crystals) is most often seen in gall bladder disease, and is thought to represent sequelae of cholestasis 1. CT chest scans showed at least two large loculations and the lower of these contained “milk of calcium” creating a fluid–fluid level with the rest of the locular contents (fig. 4 ⇑). The unusual aspect of this case is the presence of multiple rounded lesions mimicking a mediastinal mass on the chest radiograph. Serum biochemistry, liver function tests and immunoglobulins were normal.Ĭhest radiography (fig. 1 ⇓) and CT scans of the lungs and mediastinum (figs 2 ⇓–4 ⇓) were performed. 
Laboratory studies demonstrated a normal full blood count, erythrocyte sedimentation rate (ESR) of 2 and C-reactive protein (CRP) of 5 mg In the chest, dullness to percussion was noted over the left clavicle, where breath sounds were also diminished. On examination there were a few shotty axillary lymph nodes, the largest being 1.5 cm on the right medial wall. He had a 15-pack-yr smoking history and drank 10 units of alcohol per week. No further imaging of the chest was carried out until this presentation. The latter was successfully managed by thoracoscopic insufflation of 4.95 g of iodised asbestos-free talc. The patient had previously enjoyed good health, apart from developing bilateral primary spontaneous pneumothoraces, followed soon after by a recurrent left pneumothorax, 7 yrs previously. When reviewed in clinic, his constitutional symptoms had resolved, leaving only a complaint of “clicking” during inspiration. No other information was available from the hospital in the USA. He declined the intervention and returned to the UK for continued management. Subsequently, computed tomography (CT) of the thorax was undertaken and he was advised that he would need a mediastinoscopy. He attended hospital, where the unusual appearance of his chest radiograph was noted. While in the USA, 1 month previously, he became unwell, with night sweats, malaise, cough and pleuritic chest pain. In case the sample is deemed inadequate the surgeon can obtain more samples before the patient is brought out of anesthesia.A 29-yr-old male was seen in clinic for apparent mediastinal lymphadenopathy. The final diagnosis often takes five to seven days as the sample has to be processed in a particular manner and special tests carried out on it. This helps the surgeon, as the pathologist is able to indicate whether or not the sample is adequate and also is able to point to a tentative diagnosis. 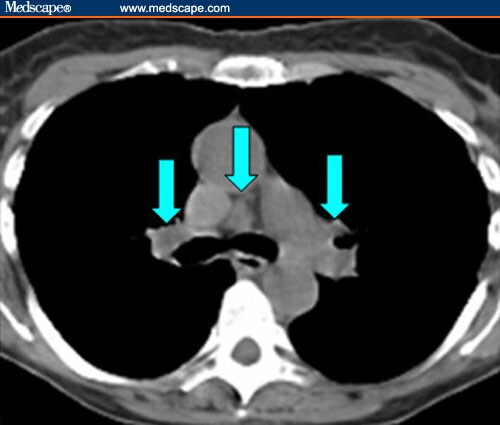
Usually the sample is sent to a pathologist immediately for processing (called frozen section) when the patient is under anaesthesia. At the end of the procedure a small tube may be placed in the chest. The surgeon then exposes the area of enlarged lymph nodes and obtains a biopsy with the help of special, long instruments introduced inside the chest through two other cannulas and by observing the picture of the operative site on the television screen. The telescope that picks up the picture of the inside of the chest and transmits it to a television screen. To look inside the chest, the surgeon passes a telescope connected to a miniature video camera through the cannula. The surgeon makes a small (about 1-cm) incision and places a short tube called a cannula in the chest. Thoracoscopic lymph node biopsy is carried out under general anaesthesia.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
